At-home HPV tests could spare millions from Pap smears
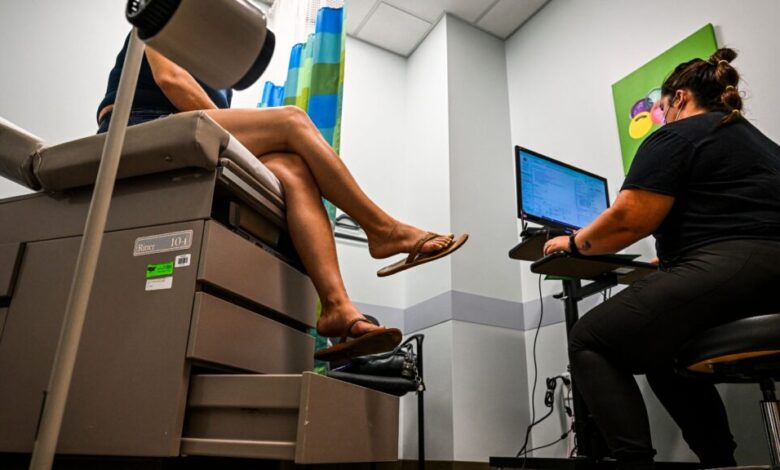
“We know that the Pap smear is not a great screen for HPV,” Doll said. “It’s not very specific, and it doesn’t really identify the thing that we know is most closely associated with cervical cancer, which is infection with HPV.”
Even before the new guidelines, the American College of Obstetricians and Gynecologists had recommended that women under 30 undergo HPV testing every five years, instead of Pap smears every three years. And while the U.S. Preventive Services Task Force still recommends Pap testing every three years for women aged 21 to 29, the HPV test is also considered acceptable.
The change is important, because the HPV test is both more sensitive and more specific than the Pap test, Doll said. “It’s more accurate in identifying women who actually have HPV that could lead to cervical cancer,” she said.
“Screening for HPV is really the gold standard for cervical cancer prevention,” said Schmeler.
What comes next?
With the new guidelines recommending at-home self-collection for HPV testing, some experts worry that women may be less likely to see a health care provider for other important aspects of preventive care.
“We still want people to come in to see their health care providers for other health maintenance issues,” Doll said. “But if we can get them in the door by offering them something that’s more comfortable or convenient for them, then I think that’s a great thing.”
As the medical community continues to adapt to new technologies and guidelines, the hope is that access to preventive care will only improve. The shift away from Pap smears as a routine screening tool for cervical cancer is just one example of how medicine is evolving to better serve patients’ needs and preferences.
Ultimately, the goal is to make preventive care more accessible, more comfortable, and more effective for everyone, regardless of their gender identity or past experiences with gynecological exams. And while the Pap smear may have been a cornerstone of preventive care for many years, the future of cervical cancer screening lies in new technologies and approaches that prioritize patient comfort and autonomy above all else.
The shift towards at-home cervical cancer screening tests has sparked a conversation about the broader aspects of women’s health that may be overlooked in traditional annual exams. Michelle Drew, the founder of the Ubuntu Black Family Wellness Collective, expressed concern that relying solely on the Pap smear for screening may lead to a neglect of other important gynecologic health issues.
Drew emphasized the importance of communicating to women that their annual exams encompass more than just cervical cancer screening. She highlighted the potential risks of skipping a comprehensive women’s health screening, such as increased rates of undiagnosed sexually transmitted infections.
The introduction of at-home HPV tests presents an opportunity for education and public health campaigns to emphasize the holistic nature of women’s well exams. Rather than focusing solely on cervical cancer screening, providers can use these tests as a prompt for patients to schedule a comprehensive gynecologic health visit.
Gynecologists and midwives now have the chance to dedicate more time to addressing their patients’ overall health needs during these visits. This shift allows for more thorough discussions and screenings for other types of cancer and health conditions that may be on the rise.
While at-home tests offer convenience, it is crucial for healthcare providers to interpret the results accurately and guide patients on the next steps. Positive HPV results do not automatically indicate cancer, underscoring the importance of proper follow-up and care coordination.
However, concerns have been raised about the accessibility of at-home tests for uninsured individuals. The cost of these tests may pose a barrier for those without insurance coverage, potentially widening existing disparities in healthcare access.
Despite these challenges, the integration of at-home HPV tests into women’s health screening guidelines presents an opportunity to enhance the overall quality of care. By emphasizing the importance of comprehensive gynecologic health exams and ensuring proper follow-up care, healthcare providers can empower women to take charge of their health and well-being.