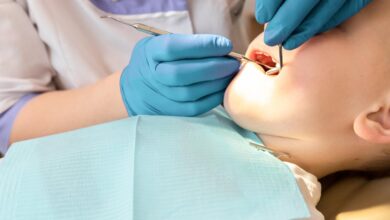
Millions could face higher ACA premiums, lower subsidies: “There will be sticker shock”
The upcoming year may bring a double blow to the 24 million individuals enrolled in Affordable Care Act (ACA) health plans. They could face significant premium increases along with a sharp reduction in the federal subsidies that help them afford coverage. Insurers are seeking higher premiums to account for rising medical and labor costs, as well as policy changes introduced by the Trump administration and the Republican-controlled Congress. The uncertainty surrounding the extension of more generous ACA tax subsidies is a key factor driving these rate proposals.
Experts warn that if the enhanced tax credits expire, many individuals may struggle to afford their premiums, leading to a potential increase in the number of uninsured Americans. Lawmakers on Capitol Hill are exploring options to mitigate the impact of subsidy reductions, as the nation heads into crucial midterm elections.
Initial filings indicate that insurers are requesting a median rate increase of 15%, a significant jump from previous years. Premiums are expected to vary based on location, plan type, and insurer. In some states, insurers are seeking increases ranging from 8.1% to 18.7%, with the average statewide increase projected to be around 7.9% if the enhanced tax credits are extended.
The expiration of the enhanced subsidies could result in a substantial rise in the average amount individuals pay for coverage, with some states seeing premiums double. Experts estimate that enrollment in ACA plans could drop by as much as 57% if the tax credits are not extended. Insurers are factoring in potential enrollment losses in their rate proposals, which could lead to higher costs for those who remain enrolled.
Discussions are ongoing in Congress regarding the extension of subsidies, with some lawmakers considering alternative scenarios to address the issue. However, any changes to the subsidy structure are likely to face opposition. While some argue that the enhanced subsidies have been prone to abuse, others emphasize the importance of maintaining assistance for individuals who rely on it.
Allowing the enhanced subsidies to expire could have far-reaching consequences, potentially reshaping the healthcare market. Some individuals may opt to drop coverage, while others may switch to plans with lower premiums but higher deductibles. The upcoming year is expected to bring significant changes to the ACA landscape, with potential implications for both insurers and consumers.