The hidden problem in emergency department STI care: Overtreating men, undertreating women
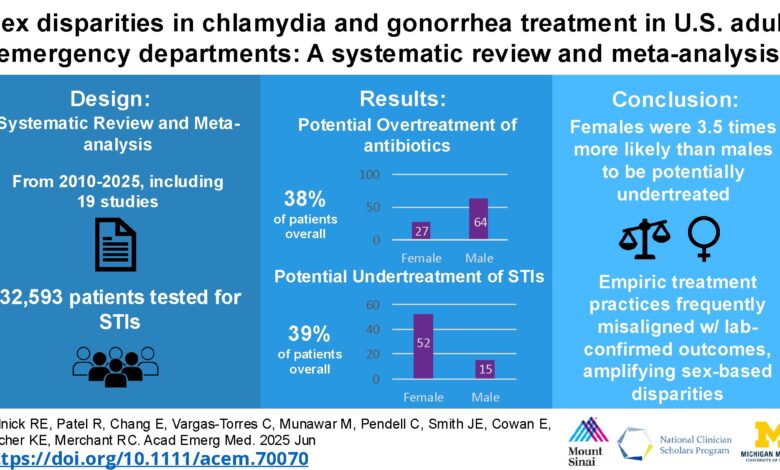
Sexually transmitted infections (STIs) are a significant public health concern, with millions of Americans affected each year. In emergency departments (EDs), the challenge of diagnosing and treating these infections is amplified by the need for quick decisions and limited information. A recent systematic review published in Academic Emergency Medicine sheds light on a troubling trend: the overtreating of men and the undertreating of women for chlamydia and gonorrhea.
When patients present with symptoms that suggest an STI, emergency department healthcare providers often face a dilemma. Should they administer antibiotics immediately, without waiting for lab results, or risk the patient not returning for treatment if the results come back positive? National guidelines tend to lean towards empiric treatment, leading to a concerning statistic revealed in the review. It was found that 38% of ED patients who ultimately tested negative for chlamydia or gonorrhea still received unnecessary antibiotics.
Furthermore, the review uncovered a significant gender disparity in STI care. Women were found to be undertreated for STIs far more often than men, with more than half of positive cases in women lacking documented treatment. On the other hand, men were more likely to be overtreated, receiving antibiotics even when test results were negative. This imbalance highlights the need for a reevaluation of how EDs diagnose and treat these common bacterial infections.
Chlamydia and gonorrhea can have serious consequences if left untreated, particularly for women who are at risk of pelvic inflammatory disease, infertility, and chronic pelvic pain. With STI clinics closing and primary care access strained, emergency departments have become crucial in providing STI care. However, the current approach may contribute to antibiotic resistance, unnecessary side effects, and increased medical costs.
To address these issues, several strategies can be implemented. Rapid molecular tests that provide real-time results for chlamydia and gonorrhea are one solution that could help avoid unnecessary antibiotic treatment. Shared decision-making with patients, ED callbacks for follow-up care, and integrating clinical decision support into electronic health records are other approaches that could improve the quality of STI care in emergency departments.
In conclusion, the review highlights the importance of recognizing and addressing disparities in STI care in the emergency department. By implementing evidence-based practices, using innovative diagnostic tools, and focusing on equity, healthcare providers can deliver more personalized and effective care to all patients. Every shift in the ED is an opportunity to make a difference and reduce avoidable harm, ensuring that STI care is not only fast but also fair and equitable for all individuals.