New Medicaid eligibility rules may reduce lifesaving cancer screenings
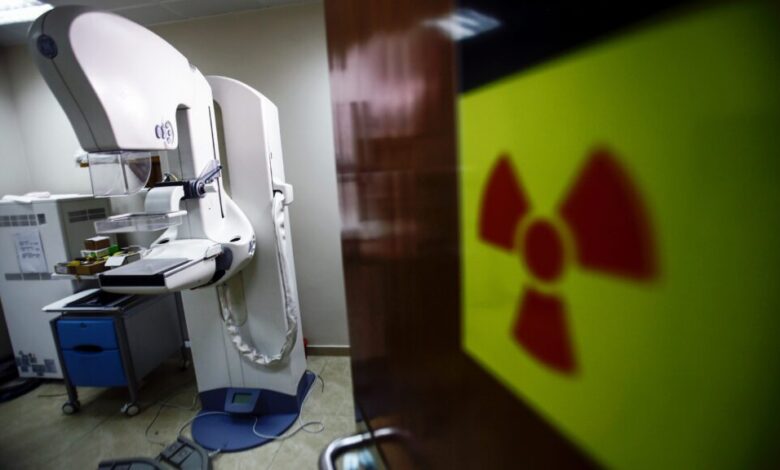
Medicaid is a vital lifeline for millions of Americans, providing access to essential healthcare services like cancer screenings. However, new eligibility restrictions set to go into effect in less than a year may cause many people to lose their coverage, putting them at risk of missing potentially life-saving screenings such as colonoscopies or mammograms. A recent analysis published in JAMA Oncology estimates that over a million cancer screenings for colorectal, breast, or lung cancer could be missed in the two years following the implementation of the new policy.
Dr. Adrian Diaz, a surgical oncologist at the University of Chicago and one of the authors of the study, expressed concern over the potential impact of the Medicaid cuts. He emphasized the importance of early cancer detection through screening, highlighting that catching cancer in its early stages can make it more treatable and curable. The analysis predicts that the new Medicaid eligibility requirements, including work requirements and re-verification of eligibility every six months, could lead to nearly 1.2 million missed cancer screenings and 155 preventable deaths within two years.
The One Big Beautiful Bill, which includes an estimated $1 trillion in Medicaid cuts, was signed into law by President Trump on July 4th last year. Republicans argued that the cuts were necessary to offset the cost of tax cuts and rein in rising Medicaid expenses. However, health groups, advocates, Democrats, and some Republicans raised concerns about the potential consequences of the cuts, warning that millions of people could lose insurance and tens of thousands of preventable deaths could occur.
The researchers behind the analysis used real-world data from Arkansas, where a work requirement was implemented in 2018, and from the Covid-19 pandemic when re-verification requirements were eased, to build a model predicting the impact of the new Medicaid restrictions. They found that administrative burdens and errors, such as failing to submit proof of earnings or missing deadlines, could result in individuals losing their Medicaid coverage and subsequently missing vital cancer screenings.
In an interview with STAT, Dr. Diaz emphasized the significance of the study’s findings and the potential consequences of the policy changes. He highlighted the challenges that Medicaid beneficiaries face in navigating the complex healthcare system, especially when dealing with a cancer diagnosis. The study also projected that 155 avoidable deaths could occur due to missed screenings, underscoring the importance of timely access to healthcare services.
As the implementation date of the new Medicaid restrictions approaches, concerns about the impact on vulnerable populations continue to grow. Access to cancer screenings is crucial for early detection and treatment, and any barriers to healthcare coverage could have far-reaching consequences. It is essential for policymakers to consider the potential repercussions of these changes and work towards ensuring that all individuals have access to the care they need to stay healthy and well.





